Venous Ulcers
What are Venous Ulcers?
Venous ulcers are the most common type of leg ulcer found in humans.
They are caused by faulty valves, which in turn cause high pressure in the veins. This alters the flow of blood in the capillaries of the skin causing poor metabolism.
What are symptoms of Venous Ulcers?
Common symptoms (what patients report) and signs (what is found on examination) of venous ulcers include:
– Ulcers on the inner ankle, or below the knee (arterial ulcers are more common on the outer ankle, toes, feet and heels).
– Generally painless
– Redness, aching, inflammation, swelling and itchy skin or hardened skin
– Sometimes the skin may ooze discharge
– Sometimes there is scabbing or flaking
– Skin may be shiny and hot to the touch
– Sometimes skin may be stained black or brown
What causes Venous Ulcers?
Common causes of venous ulcers include:
– Deep Vein Thrombosis
– Varicose Veins
– Obesity
– Immobility
– Less commonly, congestive heart failure
– Venous ulcers, like most venous conditions are more common the older one is.
What is the treatment of Venous Ulcers?
Venous ulcers may take months to heal, and your doctor may recommend various strategies to decrease the venous pressure and reduce infection including:
- Antibiotics should be used rarely and with caution due to encouraging antibiotic resistance.
They should NEVER be used without dealing with the high venous pressure to heal the ulcer.
This is a common mistake. The telltale signs of infection include redness, pain around the ulcer, pus.
An uninfected ulcer generally doesn’t have the redness, tenderness and pain.
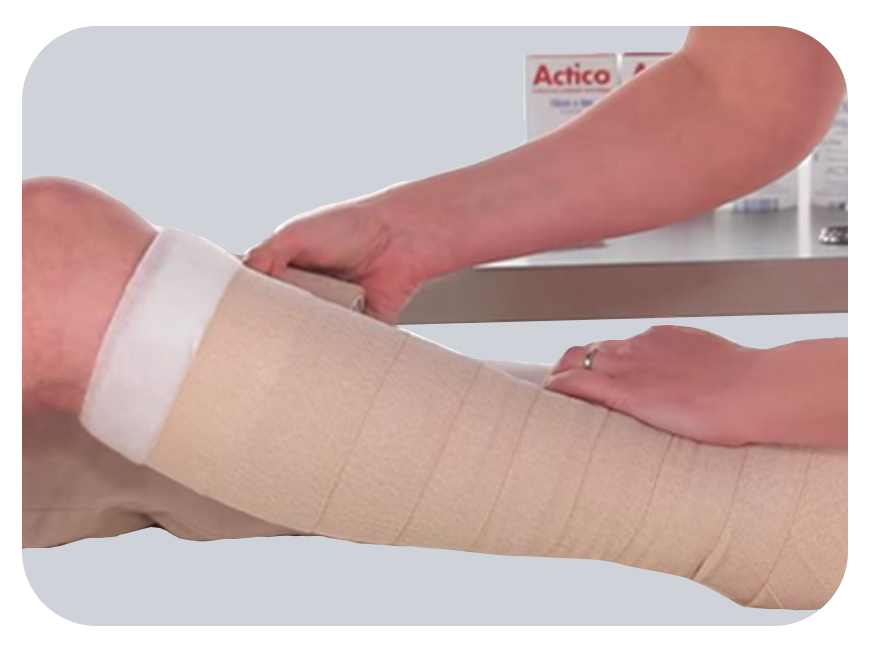
- Properly cleaning and bandaging the wound.
- Dressings should be changed weekly or more often if necessary (if dressing becomes wet or is odorous). Ulcers heal faster when covered.
- Compression bandages to control venous pressure.
- Painkillers to reduce pain
- Leg elevation on a pillow is only helpful if compression is difficult or not possible